Platelet-Rich Plasma (PRP) for Joint, Tendon, and Ligament Injuries: A Regenerative Approach to Musculoskeletal Healing
How ultrasound-guided platelet-rich plasma (PRP) injections work, the science behind autologous regenerative therapy, and how ReGenesis uses PRP for tendon, ligament, and mild-to-moderate arthritic joint conditions.
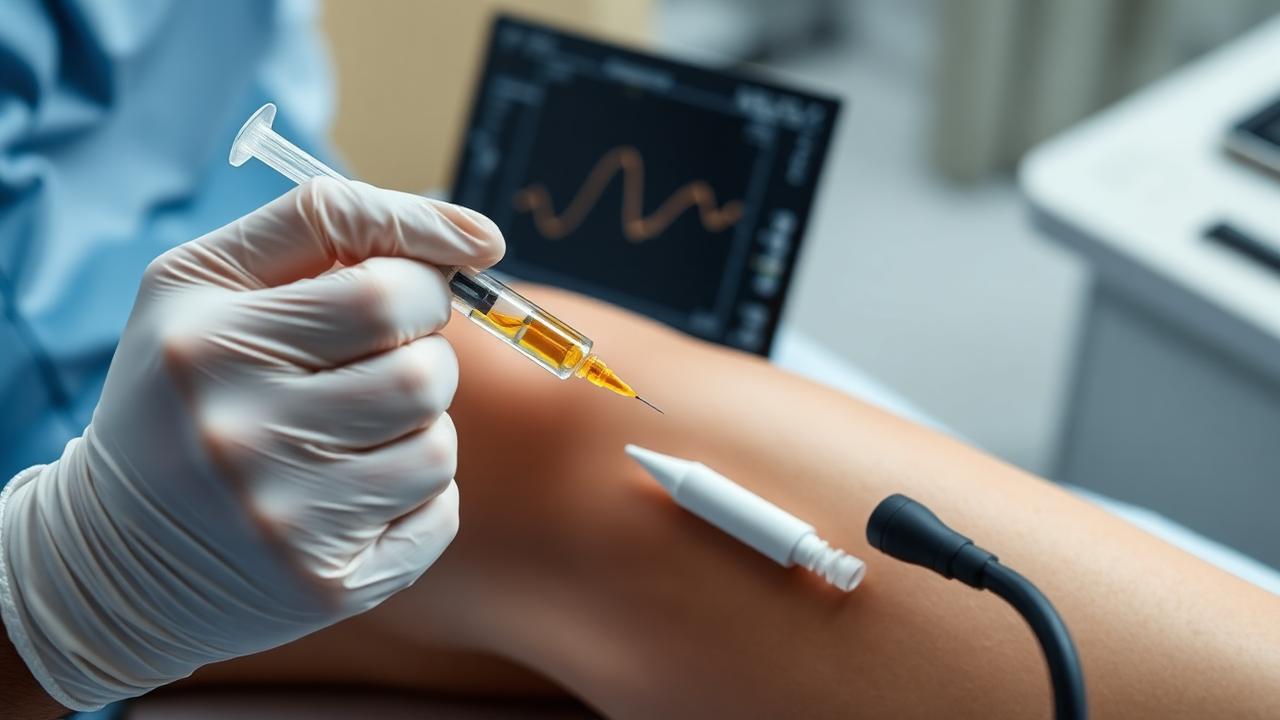
Joint, tendon, and ligament injuries are among the most persistent challenges in musculoskeletal medicine. Whether the issue is a chronically irritated rotator cuff, a stubborn case of tennis elbow, a partially torn ligament, or a knee that has slowly developed mild-to-moderate osteoarthritis, the conventional pathway often follows a familiar pattern: anti-inflammatory medications, physiotherapy, corticosteroid injections, and — when the pain returns — a discussion about surgery. For a meaningful subset of these patients, there is an evidence-supported intermediate option that addresses the underlying biology of the injury rather than simply masking the inflammation: platelet-rich plasma, or PRP.
At ReGenesis Longevity Clinic™, ultrasound-guided platelet-rich plasma is one of the core regenerative tools used to treat tendon, ligament, and select arthritic joint conditions. Delivered with image guidance, supported by a structured assessment, and integrated into a broader rehabilitation plan, PRP becomes far more than just an injection — it becomes a precise biological intervention.
What Is Platelet-Rich Plasma (PRP)?
Platelet-rich plasma is an autologous (from your own body) concentrate of platelets and growth factors prepared from a small sample of the patient's own blood. After a venous draw, the blood is processed in a centrifuge to separate red blood cells from plasma and to concentrate the platelets several-fold above their normal physiological level. The resulting platelet-rich plasma is then injected — under ultrasound guidance — directly into the injured tendon, ligament, or joint.
Platelets are far more than clotting cells. They are dense reservoirs of bioactive growth factors and cytokines, including platelet-derived growth factor (PDGF), transforming growth factor-beta (TGF-β), vascular endothelial growth factor (VEGF), insulin-like growth factor (IGF-1), epidermal growth factor (EGF), and fibroblast growth factor (FGF). When platelets are concentrated and delivered into damaged tissue, these growth factors are released in high local concentration, initiating a cascade that promotes cellular proliferation, matrix synthesis, angiogenesis, and tissue remodeling.
Why Ultrasound Guidance Matters
PRP delivered without imaging guidance is a blind injection — and in tendons, joint capsules, and small ligamentous structures, blind accuracy is poor. Ultrasound guidance allows the clinician to visualize the target tissue in real time, advance the needle to the exact pathology (a hypoechoic tendon lesion, a partial tear, an enthesis, or an intra-articular space), confirm placement, and observe the injectate distributing along the intended structure. This precision is what separates effective regenerative practice from a hopeful injection.
The Science Behind PRP
PRP works by amplifying — not replacing — the body's natural repair biology. The mechanism unfolds in overlapping phases that mirror normal wound healing, but at a higher intensity and in tissues that often have poor intrinsic healing capacity (such as tendons and the inner two-thirds of menisci).
1. Growth Factor Release and Cellular Recruitment
Within minutes of injection, activated platelets degranulate and release their stored growth factors. PDGF and TGF-β recruit and activate fibroblasts and tenocytes; VEGF stimulates new blood vessel formation in poorly vascularized tissue; IGF-1 promotes cell proliferation; and EGF and FGF support epithelial and mesenchymal cell activity. The combined effect is a localized, high-intensity signaling environment that triggers a coordinated repair response.
2. Matrix Synthesis and Tissue Remodeling
Over the following weeks, recruited fibroblasts and tenocytes synthesize new type I and type III collagen, proteoglycans, and other extracellular matrix components. In tendons, this means restoration of organized collagen architecture; in ligaments, improved tensile strength; in joint capsules, more competent connective tissue support. Maturation and cross-linking continue for months after the injection, which is why the full clinical response to PRP is typically not seen for 8 to 12 weeks.
3. Modulation of Inflammation and Pain Signaling
PRP also influences the local inflammatory and pain environment. It modulates cytokine balance, reduces chronic pro-inflammatory signaling characteristic of tendinopathy and degenerative joint disease, and appears to downregulate peripheral pain pathways. In mild-to-moderate osteoarthritis, intra-articular PRP has been shown in multiple randomized controlled trials to reduce pain and improve function — often more durably than corticosteroid or hyaluronic acid injections.
What the Evidence Says
The PRP literature has matured considerably over the past 15 years. The strongest evidence supports its use in lateral epicondylitis (tennis elbow), patellar and Achilles tendinopathy, rotator cuff tendinopathy and partial tears, plantar fasciitis, mild-to-moderate knee osteoarthritis, and selected ligamentous injuries. Multiple meta-analyses have shown durable benefit for knee osteoarthritis at 6 and 12 months, often outperforming hyaluronic acid and corticosteroid in head-to-head comparisons. As with all regenerative therapies, results depend heavily on patient selection, image guidance, preparation protocol, and an appropriately structured treatment course.
Indications: When PRP Makes Clinical Sense
PRP is most effective when there is biological tissue to repair — that is, an injury or degenerative process that is partial rather than complete, and a patient whose general health supports a robust healing response. The strongest candidates share a common pattern: persistent musculoskeletal pain or dysfunction with imaging or clinical evidence of tendinopathy, partial tearing, ligamentous compromise, or mild-to-moderate joint degeneration.
Tendon Injuries (Tendinopathy and Partial Tears)
Chronic tendinopathy of the rotator cuff, common extensor origin (tennis elbow), common flexor origin (golfer's elbow), patellar tendon, Achilles tendon, gluteal tendons, and plantar fascia all respond well to ultrasound-guided PRP in appropriately selected patients. Partial-thickness tears, when not large enough to require surgical repair, are particularly good candidates because PRP can stimulate the kind of structured collagen remodeling that tendons cannot reliably achieve on their own.
Ligament Injuries
Partial ligament injuries — including medial collateral ligament sprains, ankle ligament injuries, ulnar collateral ligament strains, and select spinal and pelvic ligamentous laxity — can benefit from PRP. The treatment promotes collagen remodeling and improved tensile strength, often allowing patients to return to activity with less risk of recurrent injury than with rest and rehabilitation alone.
Mild-to-Moderate Arthritic Joints
Mild-to-moderate osteoarthritis is one of the most well-supported indications for intra-articular PRP. In knees, hips, shoulders, and small joints showing mild-to-moderate degenerative change (typically Kellgren-Lawrence grades 1 to 3), PRP can reduce pain, improve function, and modulate the chronic inflammatory environment that drives ongoing cartilage breakdown. PRP does not regrow cartilage in any structurally meaningful way, and it is not a substitute for joint replacement in advanced disease — but for patients in the mild-to-moderate range, it often delays progression and meaningfully improves quality of life.
Other Indications
PRP has also been used for plantar fasciitis, hip labral irritation, sacroiliac joint dysfunction, certain spinal conditions, and aesthetic and sexual health applications. At ReGenesis, our musculoskeletal PRP focus is on tendon, ligament, and mild-to-moderate arthritic joint conditions. Other applications can be considered, but each requires an individualized assessment to determine whether PRP is the right tool, whether another regenerative approach (prolotherapy, hydrodissection, hydro-dilation) is more appropriate, or whether a different pathway is indicated.
What to Expect at ReGenesis
A PRP program at ReGenesis Longevity Clinic™ begins with a thorough clinical evaluation — history, physical examination, review of any prior imaging, and a focused musculoskeletal ultrasound assessment of the target structures. This step is essential. Without a clear understanding of which tissue is responsible for the symptoms and how much structural compromise is present, no injection — regenerative or otherwise — can be expected to deliver consistent results.
The Procedure Itself
Each PRP visit takes approximately 60 minutes. A small volume of blood is drawn from a vein in the arm and processed in a centrifuge in the clinic to concentrate the platelets. While the PRP is being prepared, the treatment site is cleaned and a sterile field established. Using high-frequency ultrasound, the target tendon, ligament, or joint is visualized in real time, and a fine needle is advanced under direct visualization to the precise pathology. The PRP is then delivered. Most patients describe the procedure as briefly uncomfortable rather than painful and walk out under their own power.
After the Procedure
Mild post-injection soreness and stiffness for 2 to 5 days is expected and is part of the mechanism — PRP intentionally initiates a healing cascade, and a brief inflammatory response is part of that. Patients must avoid all non-steroidal anti-inflammatory medications (NSAIDs) — such as ibuprofen, naproxen, and aspirin — for the duration of the treatment course, as NSAIDs blunt the very biological response PRP is designed to trigger. Acetaminophen, ice for short periods if needed, gentle range-of-motion work, and adequate hydration are recommended for symptom management. Activity modification for the first 1 to 2 weeks is typical, followed by a graduated return to loading and rehabilitation.
Treatment Series and Realistic Timelines
PRP protocols are individualized. Some patients will respond well to a single treatment, while others may require up to 3 treatments spaced at 6-week intervals to achieve durable improvement, followed by a single maintenance treatment per year. The number of sessions depends on the tissue treated, the chronicity and severity of the injury, the patient's overall biological response, and the goals of care. Meaningful improvement is typically appreciated by 6 to 12 weeks after each treatment, with continued maturation of the repair tissue over several months. Concurrent rehabilitation — progressive loading, motor control work, and activity modification — is strongly encouraged to consolidate the biological gains.
Cost of Treatment
At ReGenesis Longevity Clinic™, ultrasound-guided PRP is offered at $550 for a single-site treatment and $900 when a second site is treated during the same visit. Prices are subject to change. The total cost of a complete program will depend on the number of sites treated, the number of sessions required, and whether annual maintenance is recommended — all of which are determined during your initial assessment.
Who Is Not a Good Candidate?
PRP is not appropriate for every patient. Active local or systemic infection, active malignancy at the treatment site, certain blood disorders, severe thrombocytopenia, anticoagulation that cannot be safely held, and patients with complete tendon ruptures or end-stage joint destruction are generally not suitable candidates. Patients on chronic NSAIDs who are unable to discontinue them, those with unrealistic expectations of a single-session cure, or those whose pain is primarily neuropathic in origin are also unlikely to benefit. A careful upfront assessment is what allows us to say honestly whether PRP is — or is not — the right tool for a given patient.
How PRP Fits Within ReGenesis' Regenerative Program
PRP is one option within a broader regenerative musculoskeletal program at ReGenesis. Depending on the clinical picture, we may recommend PRP alone, ultrasound-guided prolotherapy, hydrodissection for nerve entrapment, hydro-dilation for adhesive capsulitis, or a combination tailored to the specific pathology. The choice is driven by the diagnosis and the tissue we are trying to influence — not by a one-size-fits-all protocol. In some patients, a sequenced approach (for example, prolotherapy to address ligamentous laxity followed by PRP to support tendon healing) produces the most durable result.
If you are dealing with a persistent tendon, ligament, or joint problem that has not resolved with conventional care, a focused assessment is the right next step. Our team will determine whether ultrasound-guided PRP is an appropriate option for you, what realistic outcomes look like in your specific case, and how the treatment should be integrated with rehabilitation and the rest of your care.
Book a Regenerative Medicine Assessment
To learn more about ultrasound-guided platelet-rich plasma at ReGenesis Longevity Clinic™, or to discuss whether you are a candidate for PRP treatment of a tendon, ligament, or arthritic joint condition, please book a consultation or visit our Regenerative Medicine Edmonton and Regenerative Medicine Calgary program pages. You may also be interested in our companion article on ultrasound-guided prolotherapy for back pain and SI joint instability.